Category: Interviews
-
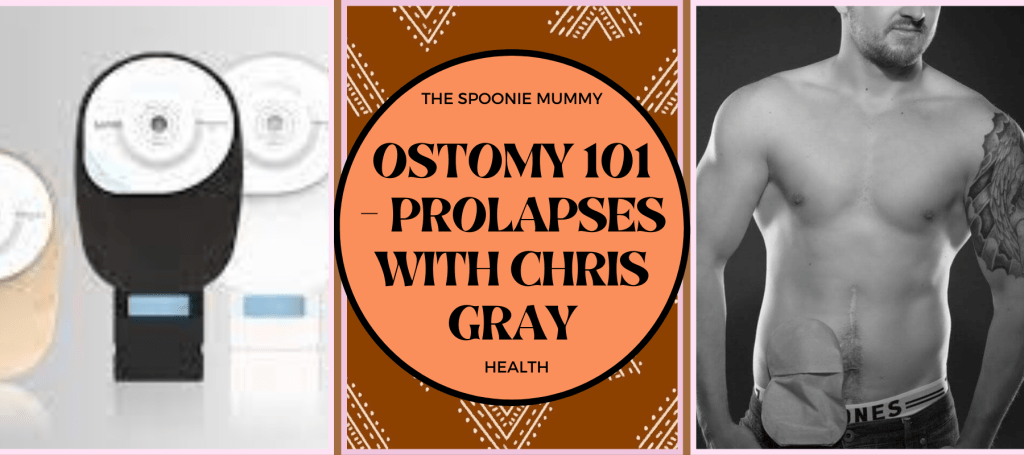
Ostomy 101 – Prolapses with Chris Gray
TW – There are pictures of a stoma prolapse included in this post. I am not a medical professional – please see your specialist if you are experiencing issues with your ostomy. What is a Prolapsed Stoma? Sometimes, the bowel can extend in length from the stomal opening – anywhere from 2-3cm to over 10cm.…
Written by
·
-

An Interview With… Danny Callaghan AKA DC vs UC
Happy new year! I hope everyone reading had a lovely Christmas and Covid didn’t spoil too many plans! I had a fab time with the boys and other family members – as my Aunty and Uncle had come down with Covid we also saw the return of the video chat family quizzes which were a…
Written by
·
-

An Interview With Lisa Kate Ostomate
Another day, another blog post! Yesterday was #ostomyawarenessday and you may have seen me posting about this lots on my social media. It was fantastic seeing so many ostomates sharing their stories, photos and information about their ostomies, why they have them and what it means to them. Lisa is someone I first started chatting…
Written by
·
-

World lupus day – an interview with amber from the world sees normal
Today is World Lupus Day and s it is a disease which has some similarities with Rheumatoid Arthritis, I thought it would be a great opportunity to find out more about it. Through the amazing Chronic Illness Bloggers network I have met people who blog about all different health conditions and discovered Amber’s blog, The…
Written by
·
-

Disabled Access Day 2020 – An Interview with Bex from ‘The Unicorn Mummy’ blog
I have said it before and I will say it again- although social media has its dark sides, it has introduced me to a group of AMAZING people and that includes today’s interviewee. I met Bex in an Instagram parents group. As a fellow disabled parent I obviously was drawn to her account and have…
Written by
·
-

Dating With IBD/Stomas – The Good, The Bad and the Smelly!
Ad | Sponsored Happy Valentines Day lovely readers! I am not a huge celebrator of this day but I had to mark the occasion as it is always a good idea to spread some more love in my opinion. I have teamed up with the fab people at Gutsy Dating for this post and am…
Written by
·
-
Deep Vein Thrombosis Awareness Month
March is national Deep-Vein Thrombosis Awareness Month, a public health initiative aimed at raising awareness of this commonly occurring medical condition and its potentially fatal complication, pulmonary embolism. What is Deep Vein Thrombosis (DVT)? DVT is a blood clot which develops in one of the deep veins in the body – usually in the leg What…
Written by
·
