As you may know, I have recently had a bit of an extended break from blogging due to having had more surgery for my Crohn’s Disease. On Wednesday June 16th I had panproctocolectomy surgery. Many people will have no clue what that is, so I thought I would write a post explaining the ins and outs of this surgery! I am always happy to answer questions so if you have any, feel free to pop them in the comments.
What is panproctocolectomy surgery?
In April 2016 I had a right hemi-colectomy, which meant part of my small and large bowel, around where they join, was removed. My stoma was then formed from the end of my small intestine. This was due to Crohn’s Disease causing scarring and blocking up a section of my bowel.
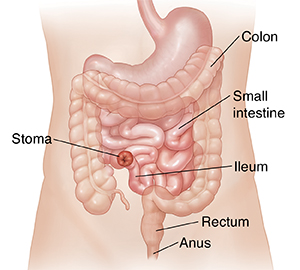
This surgery will make my ilesotomy permanent. My surgeon will remove the remaining large bowel and my rectum, then sew up my bottom – hence the nickname Barbie Butt surgery! For the guys, it either called Ken or Action Man by the way!
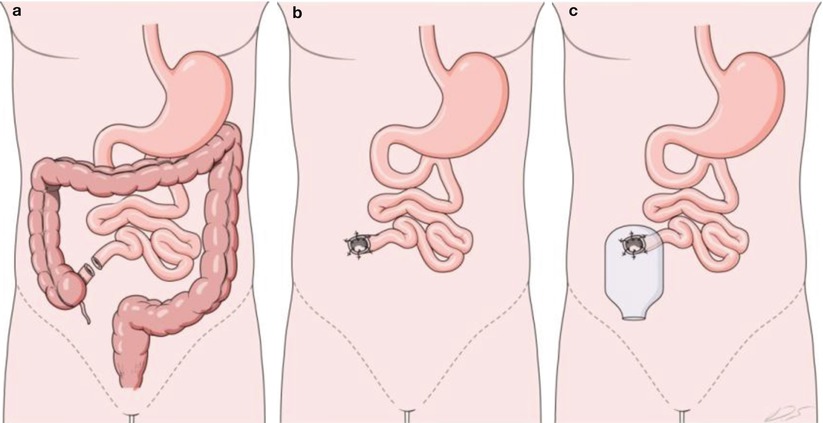
Preparing For Surgery
My hospital follow the Enhanced Recovery Plan for post surgery which actually starts before your surgery. The night before and morning of my surgery I had to drink6 bottles of Nutricia Pre Op drinks (4 in the evening and 2 in the morning) which are loaded with carbs and other good stuff to help your body through the surgery. I was dreading them to be honest, but they tasted pretty nice – just like lemon squash!

As part of the Enhanced Recovery program I was also told I would be got up out of bed and moving about as soon as possible. While this sounds hideous, it really does make a HUGE difference to your recovery.
I was told to expect to be in for 7 to 10 days so kept this in mind when packing my hospital bag. I chose to pack more nighties than I usually would, as I didn’t think I would want anything like my usual shorts laid across my scar for a little while at first. I packed some decent sanitary pads – I chose some that were soft, super absorbent and extra long as this covered the bottom area too if needed! Plenty of stoma stuff, a couple of books, toiletries, chargers, Kindle tablet and a pen and notebook all went in as usual too – if you would like me to do a more in depth post about what I pack for a hospital stay, let me know in the comments!
Telling The Boys
My boys are now 12 and 9 – and very different from the 7 and 4 olds I had when I had my ostomy surgery five years ago!
They had actually attended an appointment with me a few years ago when we first started talking about this surgery. Although they both had things to keep them busy, I could see Leo in particular listening and taking everything in. My gastro consultant is amazing and has a daughter who is a similar age to Leo so knows exactly how to word things around them so they aren’t scared or alarmed which is a huge help.
When we got out of that appointment I asked Leo what his thoughts were. I think he appreciated getting the chance to voice his opinions and his concerns – he was happy for me to keep my stoma as he appreciated how much more well I was since having it, but was worried I would be in hospital for a long time again. I explained that my ostomy surgery happened when I was very poorly and was an emergency, hence the month long stay in hospital. Making a decision about this surgery meant we could do it on our time – when I was physically well and strong, and my body was in a much better place to cope with it which would hopefully mean a shorter stay.
I had them the weekend before my surgery and I made sure they knew the next weekend I was due to have them I would probably still be in the hospital, so we would work out with Daddy when they could come as soon as I was well enough etc. I arranged for my Mum to call them the evening of surgery day to fill them in on how everything was, as I said I may not be able to chat to them straight away if I was still groggy from the op, but I would call them as soon as I was able to. Both boys bought up the possibility of me dying in surgery this time which broke my heart. I tried as best I could to allay their fears, but keep it realistic. I explained that sometimes people did die during surgery, but I wasn’t planning to as I had two of the best boys in the world to fight and wake up for. I was generally healthy so the risk was very low.
The IA have a great colouring book for children that helps explain what an ileostomy is and what happens before, during and after a surgery. While it has been created as a resource for children facing the surgery, it is a great way of explaining to your own children or grandchildren about it too. Click here to forward you to a printable version.
Surgery Plan
I saw both my surgeon and an anaesthetist before my surgery as I have an allergy to one of the anaesthetic medications so always need a review prior to any op. We discussed options for pain relief and it was decided that this time I would have an epidural placed to help manage the pain for the first few days after surgery.
I also bought up my concerns about cannulation as I am difficult to cannulate and they often blow very quickly even when they manage to get one in. It was decided that I would have a central line as well as cannulas, so they could always ensure a route to get medication in me, especially in those first few post-op days.
Covid
I had to go and have a Covid test done 3 days prior to being admitted and this was booked by my surgeon’s secretary for me. I also had a test done when I was admitted on the morning of my surgery, followed by weekly ones when I was in there.
I was also advised that no visitors would be allowed during my stay. I would not have to wear a mask while in bed, but when moving around the hospital I would be asked to wear one eg. to go for tests and scans if needed.
So that’s it – I was ready to go! Do you have any further questions about the surgery? If so please pop them in the comments and I will be back soon to fill you in on what happened next. Take care and keep safe,

Leave a comment